Flu season is upon us. This brings up important questions for many people. This is because there are a great number of misconceptions about both the flu and its vaccination. Should you get the vaccine? Will you get the flu even after you have had the vaccine? Questions like these are common among those who live in areas in which the flu virus is prevalent. The flu is a common illness, but it is not one to be taken lightly. Influenza does, in fact, causes a pandemic every year. This is the case even in countries with advanced medical access like the USA. Furthermore, complications in treatment or further illness spurring from the original infection can cause more deaths to be added to the toll each year. With such a dangerous but misunderstood virus, how can we protect ourselves and those we love? The first step is understanding the virus. Once this is done, the vaccine can be understood and evaluated based on its effectiveness and manufacturing process. Influenza is a powerful virus, but we are not helpless against it.

The virus itself follows a normal virus’ life cycle. Once the virus has entered the body, it attacks specific cells. For the flu, the virus targets the epithelial cells in the respiratory tract. The virus then latches on to the plasma membrane of the cell and injects its genome into the cell. This makes the cell a host for the virus and effective factory for producing more viruses. The host cell starts producing and assembling the proteins that the virus requires. These new viruses assemble build up in the cell. Once the cell has produced enough viruses, the cell will burst, releasing the new viruses to spread to more cells in the epithelium.
The flu virus in particular is a very fluid virus in its ability to change. There are many mutations and combinations of proteins that make the flu hard to treat from year to year. In many cases, the flu virus that causes a pandemic one year is different from the one that was prevalent the previous year. The main proteins associated with influenza are hemagglutinin and neuraminidase. These proteins are transmembrane proteins that effect the identification of each virus. There are seventeen possible hemagglutinins and ten possible neuraminidases that can be incorporated into an influenza virus. This allows for a large range of influenza viruses that can be found and treated. In addition to the natural variability of the influenza virus, mutations in the genome can occur which makes the virus a different form than any form that had been previously known. The immense variability of the virus’ proteins make treating the flu very difficult, and makes it seemingly impossible to cure.
The body’s defense system automatically responds to the virus when it enters the system. This happens in the immune system through the use of antibodies. These are naturally produced by the body in response to any foreign invader. Antibodies bind to the antigenic sites of the outer-membrane proteins of the flu virus. This antigenic site is found on the hemagglutinin portion of the plasma membrane. The problem in treatment, is that antibodies will only bind to one type of hemagglutinin. This means that for each differing hemagglutinin, a new antibody must be developed by the immune system.

Over time, you will build up your immunity to multiple strains of influenza so long as a mutation does not affect the antigenic sites. This is heavily beneficial with increasing age. As people get older, the effectiveness and efficiency of the immune system decreases. This is why it is highly important to get a flu shot every year. Complications with the flu virus more commonly take place in the elderly population. Infections such as pneumonia can occur and further threaten the lives of those who are more susceptible to infection. These complications are often times what causes mortality in flu infections as opposed to the virus itself.
The vaccination works by forcing your body to develop antibodies for a specific hemagglutinin antigen site. This is done by presenting the immune system with the virus in advance to build up antibodies. This can come in the form of an inactivated virus, or in an attenuated virus, meaning you may or may not be receiving an active version of the virus. In either case, the virus is modified to advance immunity without causing illness. The vaccination often times includes viruses from multiple strains of the flu to build immunity even further. With each vaccination, immunity for multiple strains of the virus is developed. However, the vaccination takes about two weeks to fully develop immunity in the body.
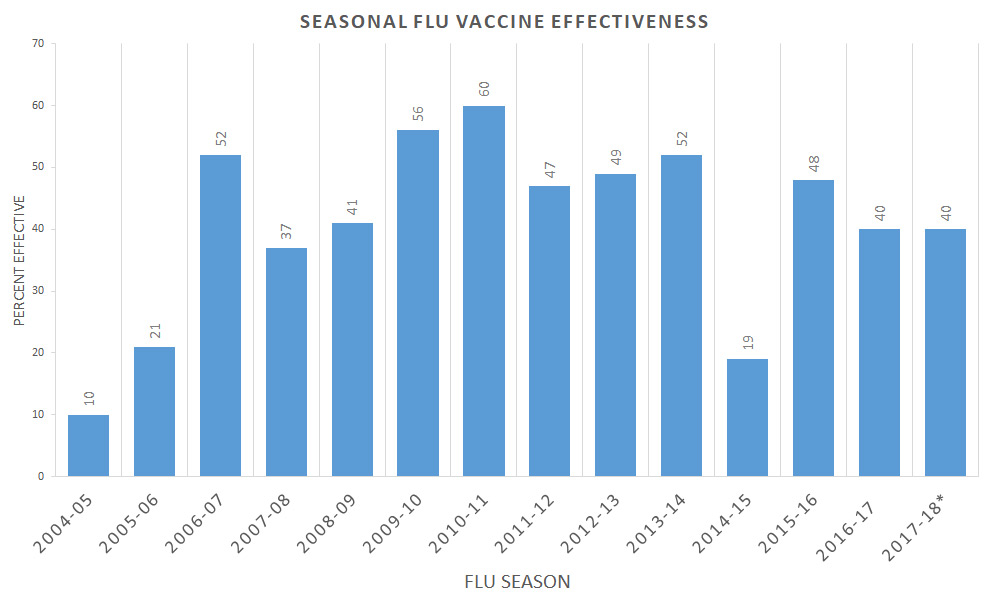
The trouble in predicting the virus breakout is that there are so many combinations of hemagglutinin and neuraminidase. Each of these combinations effect which antigens are needed for neutralization of the impending pandemic. While there are many factors that scientists take into account when predicting the next flu outbreak, there is no way to be one-hundred percent sure that they have chosen the right one. Even if the prediction for the outbreak is inaccurate, the shot is still beneficial for building immunity for future virus outbreaks.
Many misconceptions about the flu vaccine come from those who have received the vaccine and then developed an influenza infection anyway. This is primarily caused by the imprecise predictions of the scientists that year. It is also a possibility that they are in a minority that got a strain that was not covered in the vaccine. Despite many concerns, there is no reason not to get a shot. In receiving a vaccination, you are building your own immunity to flu strain, even if it is not the one that breaks out that year. Receiving the shot also protects those around you. The Influenza virus is responsible for upwards of 35,000 deaths each year in America alone [2]. By choosing to get a shot, you take a step towards preserving the health of those around you as well as your own. Influenza is a widely varied virus, but steps can be taken to protect ourselves and others from its detrimental effects.
References
- Brook, Deadly ‘Australian flu’ infecting thousands in UK (2018).
- Kim, Are We Prepared for the Next Pandemic Flu Virus? (2013).
- Centers for Disease Control and Prevention, Disease Burden of Influenza (2018).
- Centers for Disease Control and Prevention, Antigenic Characterization (2017).
- Centers for Disease Control and Prevention, Seasonal Influenza Vaccine Effectiveness, 2004-2018 (2018).
- Affelt, 5 Myths About the Flu Virus (2018).
- Maron, Beyond the Flu Shot (2018).
- Beil, One and Done (2017).
- Perry, Flu Fighters Building a Better Shot (2018).
- Leslie, Why last year’s flu vaccine didn’t work so well (2015).
- Cohen, A Once-in-a-Lifetime Flu Shot? (2013).
- Cohen, Nasty U.S. flu season continues to intensify (2018).
- Vogel, Blocking Flu at Its Core (2001).
- Centers for Disease Control and Prevention, Influenza (Flu) (2018).
- Centers for Disease Control and Prevention, Influenza A Subtypes and the Species Affected (2018).
- Centers for Disease Control and Prevention, How the Flu Virus Can Change: “Drift” and “Shift” (2017).
- Riel, V. Munster, E. de Wit, G. Rimmelzwaan, R. Fouchier, A. Osterhaus, T. Kuiken, Human and Avian Influenza Viruses Target Different Cells in the Lower Respiratory Tract of Humans and Other Mammals (2007).
- Centers for Disease Control and Prevention, Key Facts About Seasonal Flu Vaccine (2018).
- Özaltin, O. Prokopyey, A. Schaefer, M. Roberts, Optimizing the Societal Benefits of the Annual Influenza Vaccine: A Stochastic Programming Approach (2011).
- Funk & Wagnalls New World Encyclopedia, Antigen (2017).
- Cohen, Llama Antibodies Inspire Gene Spray to Prevent all Flus (2018).